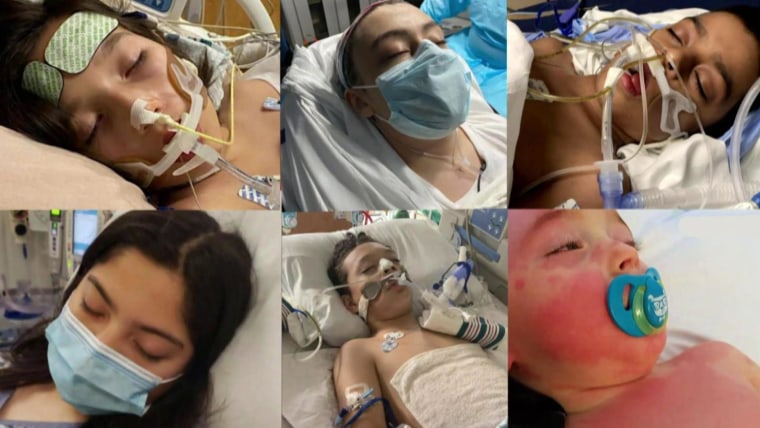
For people recovering from COVID-19, home care can be both essential and elaborate, involving a health care professional who provides additional oxygen, monitors vital signs, administers medication and helps with daily tasks such as eating, bathing and getting in and out of bed.
Home care professionals and nurses said the coronavirus pandemic shows how crucial the industry is. It provides life-saving services to people who are vulnerable while keeping them safe in their own homes.
“It’s been quite a dramatic challenge for all of us and certainly the public health challenge of our lifetime,” said Dr. Steven Landers, president and CEO of the Visiting Nurse Association Health Group, which serves New Jersey and Ohio.
“Nurses, therapists, home health aides, they have really shown up to help fragile, medically vulnerable people stay home and also help people come home from hospitals and nursing homes, which have been under incredible stress,” he said.
Landers said his organization has helped more than 500 patients in New Jersey with home services get out of hospitals and emergency rooms. The workers have adapted to the pandemic, learning new protocols and infection control regimens and wearing new types of protective equipment, he said.
Olga Jarrín, a registered nurse and assistant professor in nursing science at Rutgers University, said there is often a lack of public awareness about what home care is and who can benefit from it. “It can be so many different things,” she said.
There are “three big buckets” of home care, Jarrín said: the short-term, immediate care a person may receive after they leave a hospital and need additional treatment; monitoring and management of a chronic illness over time; and palliative care.
Home care also includes a broad range of medical and personal services for people who need assistance in the home. That can include help with daily living needs, such as services provided by a home health aide, as well as medical needs provided by medical professionals, such as nurses or therapists.
Home care can include personal daily tasks such as help with medications, bathing and turning to prevent bed sores. It can also include medical care such as taking care of wounds, administering infusions and injections, providing physical therapy, managing and monitoring vital signs and other medical interventions.
Vicki Hoak, executive director of the Home Care Association of America, said the coronavirus pandemic has “absolutely changed the face of home care” and “upended everything about our daily operations.”
“I think it’s caused us all to think about our mission, the way we deliver the care, the way we communicate and how we’re regarded by other partners in the health care communities,” she said. “My hope is that absolutely more light has been shed on this valuable workforce.”
Let our news meet your inbox. The news and stories that matters, delivered weekday mornings.
Home care employees are also critical front-line workers in the fight against coronavirus, Hoak said, and face similar issues hospitals face, such as the initial lack of life-saving personal protective equipment. Such equipment is essential to protect patients the home care workers serve every day and to protect themselves, she said.
“We deliver care in people’s private homes. We’re kind of like the invisible care provider,” she said. “We see any change of condition and we can monitor and we can keep people safe.”
Jarrín said one recent positive change to home care is allowing nurse practitioners and physician assistants to order home health care services for Medicare patients through the CARES Act.
“Some of the restrictions on practices have been really opened and are going to benefit patients and the home health care teams that have been working against these limitations,” she said.
She said there could also be an influx of experienced nurses coming into home health care.
“I think there’s going to be a huge, growing demand. This has been the fastest-growing need for home care services,” she said. “I think we’re going to see a tremendous growth.”
Warren Hebert, chief executive officer of the HomeCare Association of Louisiana, said he also believed there would be increased skilled nursing in the home setting, as well as more community-based services and more palliative and hospice care in the home.
Hebert said families might begin seeking out additional home care options and maintaining independent living at home following reports of how coronavirus spread widely in nursing homes and other facilities. According to data collected by NBC News, at least one-third of the 90,000 known coronavirus deaths in the United States are linked to nursing homes and other long-term care facilities.
“I think that we’re going to see families thinking much harder and having much more conversation about whether that’s the right choice or not,” he said.
Hebert said in light of the pandemic and fears of infectious diseases, going forward “we need to be more intentional about the way we go about building the relationship between the health care provider and the patient and the patient’s family.”
Some families have been refusing home visits from a nurse or therapist because of those fears, he said, so it was critical for providers to communicate protocols and ensure the safety of their patients.
“That home health nurse needs to find the way to build trust and confidence with the patient and their family,” he said. “If that nurse can help to manage the person’s chronic illness well, then it keeps them out of the hospital or an urgent care center or the emergency department.”
Roger Noyes, director of communications for the Home Care Association of New York State, said the “pandemic has really required all sectors of health care to rethink everything.”
“For home care, that includes everything from basic supply issues to the role of technology in providing care,” he said.
Noyes said in New York City, home care providers have long employed telehealth monitoring and a range of telecommunication systems that have been important in keeping patients safe during a pandemic.
But to date, Noyes said, that has not been covered by Medicare.
“So, it’s really important for the federal government to follow the trend on where telehealth is going and the need to reimagine elder care services in a way that employs telehealth systems to help patients at home,” he said. “We’re finding that telehealth is vital for reducing exposure in a time of crisis like this.”
Beyond medical services, video technology is providing much-needed mental and social services during a time when so many have been isolated from their loved ones, Noyes said.
Noyes said they have received a grant to work with a home care agency called Selfhelp Community Services in New York City to build an onlinesenior center with interactive, video-based live classes for home care providers to offer their patients statewide. It will provide older adults a chance to interact with each other while learning about a variety of topics such as music, history and the arts through partnerships with institutions such as museums.
“Everyone who is experiencing this crisis knows that social Isolation is a way of life right now for all of us to some degree, and we also know technology has become a major bridge for that type of connectivity we yearn for in this moment of crisis,” Noyes said.
Russell Lusak, Selfhelp’s chief operating officer, said the virtual senior center provided social interaction for older adults during a time of extreme social isolation and depression.
“That connection to other people is so important,” he said. “It’s a great option for people that otherwise wouldn’t have the ability to go to a senior center. It’s such an incredible thing to see.”